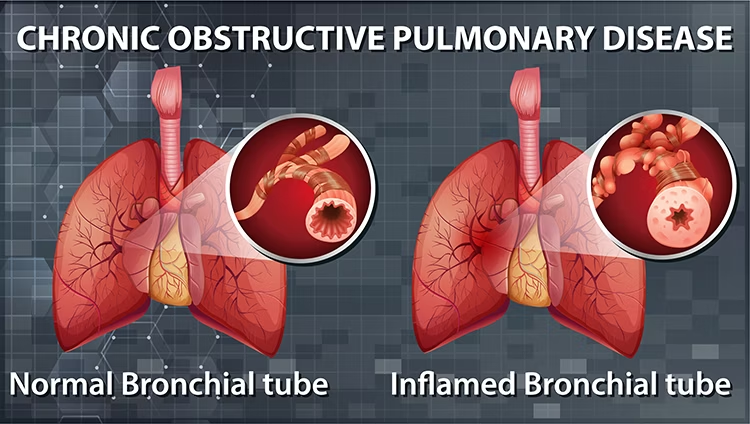
COPD: A Comprehensive Guide to Living with Chronic Lung Disease
Welcome to this comprehensive guide about COPD, a chronic lung disease that affects millions worldwide. This article is designed to provide you with a thorough understanding of COPD, its causes, and most importantly, how to effectively manage symptoms and improve quality of life while living with it.
Understanding COPD
What is Chronic Obstructive Pulmonary Disease?
Chronic Obstructive Pulmonary Disease, or COPD, is a progressive lung disease that makes it hard to breathe. It's like your airways are constantly inflamed and narrowed, making it difficult for air to flow in and out of your lungs. People with COPD often experience a variety of symptoms, including shortness of breath, chronic cough, and excessive mucus production. While there isn't a cure for COPD, early diagnosis and treatment options can help control symptoms and improve their quality of life.
Causes and Risk Factors of COPD
What are the causes of COPD and what increases the risk of developing it? Well, smoking is the leading cause of COPD, but long-term exposure to air pollution, fumes, and dust can also damage your lungs and increase the risk of COPD. Even secondhand smoke can put you at a higher risk for COPD. There's also a genetic condition called alpha-1 antitrypsin deficiency that can increase the risk for COPD. It's important to know your risk factors so you can take steps to prevent COPD or get an early diagnosis.
The Impact of COPD on Daily Life
Living with COPD can significantly impact your daily life. Simple activities like walking or climbing stairs can become difficult due to shortness of breath. The chronic cough and mucus can be bothersome and affect your sleep and social interactions. Exacerbations, or flare-ups of symptoms, can lead to hospitalizations and further decline in lung function. However, with personalized treatment plans, pulmonary rehabilitation, and lifestyle changes, individuals with COPD can manage symptoms and improve their quality of life, enabling them to continue living a fulfilling life. The goal of COPD care is to help individuals with COPD live their best lives.
Managing COPD Effectively
Recognizing Symptoms of COPD
Recognizing the symptoms of COPD is the first step in effectively managing COPD and maintaining a good quality of life. Common symptoms include shortness of breath, persistent cough, mucus production, wheezing, and fatigue. These symptoms can worsen over time, particularly during exacerbations. If you experience these symptoms, it is important to consult with your healthcare provider for an early diagnosis and treatment to prevent COPD and further lung damage. Recognizing symptoms early can significantly improve the effectiveness of treatment plans and overall lung health.
Diagnosis of COPD
The diagnosis of COPD typically involves a comprehensive evaluation by a healthcare provider. This may include a review of your medical history, a physical exam, and lung function tests such as spirometry. Spirometry measures how much air you can inhale and exhale, and how quickly you can exhale. Additional tests may include chest X-rays or CT scans to assess the severity of lung damage. Getting diagnosed with COPD early allows you to begin treatment options and lifestyle changes to manage symptoms and improve quality of life.
Developing a COPD Management Plan
Developing a COPD management plan is crucial for those diagnosed with COPD. Your healthcare provider will work with you to create personalized treatment plans that address your specific needs and goals. This plan may include medications such as inhalers, pulmonary rehabilitation, lifestyle modifications such as quitting smoking and avoiding air pollution, and strategies for managing exacerbations. Regular follow-up appointments are essential to monitor your progress and adjust your plan as needed. This proactive approach to managing COPD can significantly improve your quality of life and help individuals with COPD live a fulfilling life.
Treatment Options for COPD
Medications for COPD
Medications are a cornerstone of COPD treatment plans, and they help control symptoms and improve quality of life. Bronchodilators, administered through inhalers, help relax the airway muscles, making it easier to breathe. Inhaled corticosteroids can reduce airway inflammation and prevent COPD from worsening. Combination inhalers that contain both bronchodilators and corticosteroids are also commonly prescribed. In some cases, oral medications may be necessary. It's important to work with your healthcare provider to determine the most appropriate medication regimen for your specific needs and conditions like COPD.
Non-Pharmacological Treatment Options
In addition to medications, non-pharmacological treatment options play a vital role in COPD management. Pulmonary rehabilitation programs can help improve lung function, increase exercise tolerance, and teach effective breathing techniques. Oxygen therapy may be necessary for individuals with severe COPD to maintain adequate oxygen levels in their blood. Lifestyle modifications such as quitting smoking, avoiding air pollution, and maintaining a healthy weight are also important. A holistic approach to COPD care that combines medication and non-pharmacological therapies yields the best outcomes to improve your quality of life.
Emergency Treatments for COPD Flare-Ups
Exacerbations of COPD, often triggered by respiratory infections or air pollution, require prompt medical attention. Symptoms of a flare-up can include increased shortness of breath, excessive mucus production, and worsening cough. In such cases, your healthcare provider may prescribe antibiotics to treat bacterial infections or corticosteroids to reduce airway inflammation. In severe cases, hospitalization and respiratory support, such as mechanical ventilation, may be necessary. Having a plan in place for managing exacerbations is essential for preventing complications and improving outcomes for individuals with COPD and chronic lung disease like COPD.
Living with COPD
Lifestyle Changes to Improve Quality of Life
Making lifestyle changes is crucial when living with COPD to improve quality of life and manage symptoms. Quitting smoking is the most important step, as it can slow the progression of COPD and prevent COPD from worsening. Regular exercise, tailored to your ability, can improve lung function and overall fitness. Avoiding air pollution and secondhand smoke can also reduce airway irritation and prevent exacerbations. These lifestyle adjustments can significantly improve quality of life for individuals with COPD and chronic lung disease like COPD.
Nutrition and COPD
Proper nutrition plays a vital role in managing COPD. Maintaining a healthy weight is important, as being underweight can weaken your muscles, including those used for breathing. Maintaining a balanced diet rich in fruits, vegetables, and lean protein can provide the necessary nutrients for energy and immune function. Staying hydrated can help thin the mucus, making it easier to cough up and keep your airways clear. Consulting with a registered dietitian can help you create a personalized meal plan to support your overall health and lung function while living with COPD.
Support Systems for COPD Patients
Having a strong support system is essential for those living with COPD and chronic lung disease like COPD. Support groups can provide a sense of community and understanding, allowing you to connect with others who are facing similar challenges. Family and friends can offer emotional support and practical assistance with daily tasks. Your healthcare provider can also connect you with resources such as pulmonary rehabilitation programs and counseling services. Building a strong support network can help you cope with the emotional and physical challenges of COPD and chronic lung disease like COPD.
COPD Care and Ongoing Management
Regular Monitoring and Follow-Up
Regular monitoring and follow-up appointments with your healthcare provider are essential for effective COPD care. These visits allow your healthcare provider to assess your symptoms, monitor your lung function, and adjust your treatment plans as needed. Pulmonary function tests, such as spirometry, may be performed to track the progression of COPD and evaluate the effectiveness of your treatment options. Regular monitoring can help identify any potential problems early on and prevent exacerbations and the need for emergency treatment for COPD and chronic lung disease like COPD.
Importance of Pulmonary Rehabilitation
Pulmonary rehabilitation is a crucial component of COPD management. These programs are designed to improve lung function, increase exercise tolerance, and enhance overall quality of life. Pulmonary rehabilitation typically involves exercise training, breathing techniques, education on managing COPD, and counseling. Participants learn how to breathe more efficiently, conserve energy, and manage their symptoms effectively. Studies have shown that pulmonary rehabilitation can significantly reduce shortness of breath, improve exercise capacity, and reduce hospitalizations for individuals with COPD and chronic lung disease like COPD and prevent COPD from worsening.
Future Directions in COPD Treatment
Research into new COPD treatment options is ongoing. Scientists are exploring new medications, such as targeted therapies that address specific molecular pathways involved in COPD. Gene therapy and regenerative medicine are also being investigated as potential ways to repair damaged lung tissue and restore lung function. Advances in early diagnosis techniques, such as biomarkers, may help identify COPD earlier and improve treatment outcomes. These future directions offer hope for improved COPD care and enhanced quality of life for those living with this chronic lung disease like COPD and chronic obstructive pulmonary disease.
Q: What is COPD and what does it include?
A: COPD, or Chronic Obstructive Pulmonary Disease, is a chronic lung condition that includes diseases like emphysema and chronic bronchitis. It's mainly caused by long-term exposure to irritants such as cigarette smoke, dust, and chemicals that can damage the air sacs in your lungs.
Q: How can I reduce my risk of developing COPD?
A: To reduce your risk, it's best to avoid smoking and exposure to secondhand smoke. Also, try to limit your exposure to environmental factors like dust, chemicals, and pollutants. Staying active and maintaining a healthy lifestyle can help too!
Q: What are the signs of COPD and when should I see a doctor?
A: Common signs of COPD include a persistent cough, shortness of breath, and wheezing. If you notice these symptoms, especially if they worsen over time, it’s a good idea to see a healthcare professional for evaluation.
Q: Are there effective treatments for COPD?
A: Yes, there are many effective treatments available for COPD! These can include medications like bronchodilators to open the airways, corticosteroids to reduce inflammation, and sometimes lung volume reduction surgery for advanced stages of the disease.
Q: How can I manage my COPD symptoms at home?
A: You can manage your COPD symptoms by staying active, eating a balanced diet, and avoiding triggers like pollutants and cigarette smoke. Many people with COPD find breathing exercises helpful to improve their ability to breathe.
Q: What role does lung volume reduction surgery play in treating COPD?
A: Lung volume reduction surgery is an option for individuals with severe COPD. This surgery removes damaged portions of the lung, which can help improve lung function and enhance the overall ability to breathe.
Q: Can I still lead a fulfilling life with COPD?
A: Absolutely! Many individuals with COPD can lead fulfilling lives by managing their symptoms effectively. Regular check-ups with healthcare providers, staying active, and adhering to treatment plans can make a big difference.
Q: How can environmental factors affect my COPD?
A: Environmental factors like air quality, exposure to pollution, and occupational hazards can significantly impact COPD. Reducing exposure to these pollutants can help manage symptoms and improve overall lung health.
Q: What are the advanced stages of COPD like?
A: In advanced stages, COPD symptoms can be more severe, making it harder to breathe and perform daily activities. At this point, individuals may require more intensive treatments and should work closely with their healthcare team for management.
This article contains general information about medical conditions and treatments. The information is not advice, and should not be treated as such. Click here for further information.